Hormonal Acne in Central Ohio: Causes, Options, and Compounded Solutions
Estimated Read Time: 6 minutes
Blog Summary:
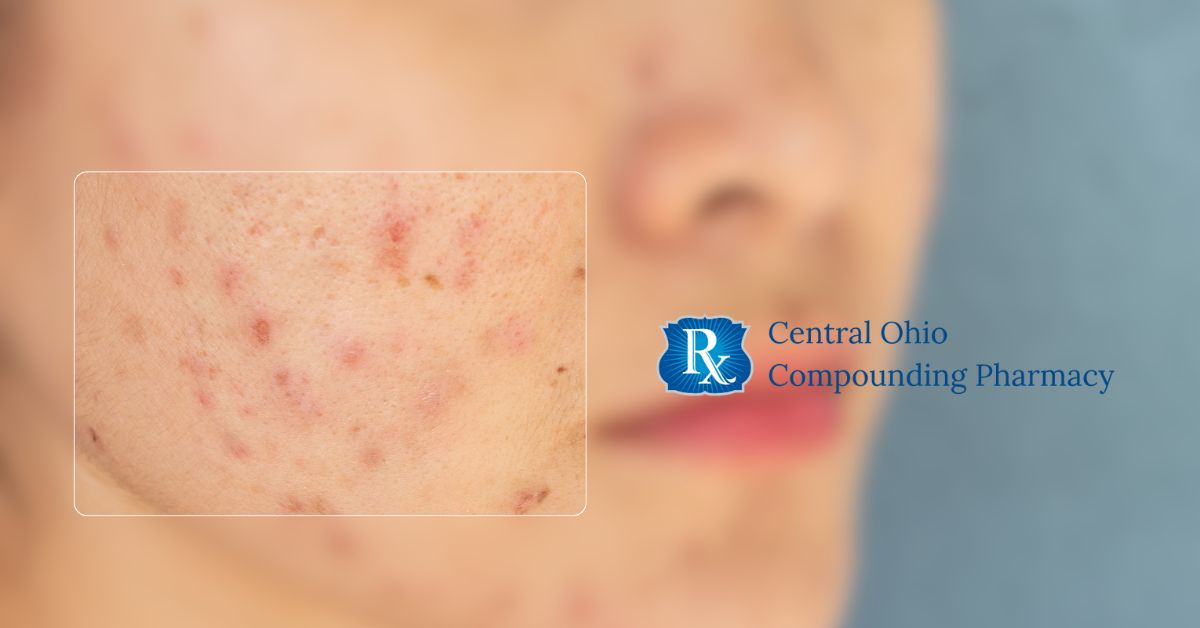
Hormonal acne in women is often addressed as a surface-level skin concern, but for many patients, the underlying cause may be more complex. Internal hormone fluctuations — particularly involving estrogen, progesterone, testosterone, and DHEA — may influence oil production, inflammation, and persistent breakouts that do not fully respond to standard therapies.
This article explores a more comprehensive approach to hormonal acne, including the role of hormone testing, personalized consultations, and bioidentical hormone replacement therapy (BHRT), alongside traditional dermatologic options. By understanding how internal hormone balance may affect the skin, patients and providers may better evaluate individualized strategies for managing hormonally influenced acne.
Hormonal acne in women is often more complex than it appears. While breakouts may show up on the skin, the underlying drivers frequently involve internal hormone fluctuations — particularly androgens, estrogen, and progesterone. These shifts may influence oil production, inflammation, and acne patterns that are often cyclical or resistant to standard therapies.
Traditional dermatology approaches — such as topical retinoids, antibiotics, or oral medications — remain an important part of care. However, for some patients, these options may not fully address the root hormonal contributors.
Because of this, some healthcare providers are exploring a broader strategy — one that includes hormone testing, individualized consultations, and bioidentical hormone replacement therapy (BHRT) as part of a comprehensive plan.
Understanding Hormonal Acne in Women
Hormonal acne most commonly appears:
- As whiteheads, blackheads, papules, pustules, or cysts
- On the jawline, chin, neck, back, or shoulders
- In cyclical patterns related to the menstrual cycle
- During hormonal transitions such as perimenopause

“Acne is the most common skin condition in the U.S. It affects nearly 80% of the population during their lifetime. About 50% of women in their 20s and 25% of women in their 40s get hormonal acne.”
Source: Cleveland Clinic
One of the primary contributors is androgen activity. Androgens — such as testosterone — may stimulate sebaceous glands, increasing oil production and contributing to clogged pores.
When androgen levels rise, the skin may respond with increased oil activity. In these situations, OTC products that focus only on the skin’s surface may offer limited benefit. Some individuals may need options that better match the underlying causes.
Several studies highlight this connection. For example, in a group of over 800 women with hormonal acne, nearly 55% showed elevated androgen levels. Another study involving 207 women with acne reported that 55% had higher levels of at least one androgen.
Because of this link, surface-level methods may not fully support those experiencing this skin condition. Without the ability to affect hormonal changes, OTC options are often unable to address what drives these breakouts.
However, acne is rarely caused by androgens alone.
The balance between estrogen, progesterone, and androgens plays a central role:
- Estrogen may help regulate oil production and increase SHBG, which binds free testosterone
- Progesterone fluctuations may influence skin behavior
- Relative androgen dominance may contribute to breakouts
Because of this complexity, identifying the underlying hormonal pattern is often a key step in developing a plan.
What Is BHRT?
Bioidentical hormone replacement therapy (BHRT) uses hormones that are structurally similar to those produced by the body. These therapies are often compounded, allowing providers to adjust:
- Dosage strength
- Hormone combinations
- Delivery methods (creams, capsules, troches, etc.)
BHRT is not a primary acne therapy, but it may be considered when acne is associated with underlying hormonal imbalance.
Why Providers May Consider BHRT for Hormonal Acne
BHRT may be considered when:
- Acne persists despite standard therapies
- Breakouts follow a hormonal pattern
- Other hormone-related symptoms are present
- Testing indicates imbalance
BHRT may play a supportive role within a broader care plan.

How Different BHRT Hormones May Relate to Acne
Estrogen: Supporting Hormonal Balance and Skin Regulation
Estrogen plays an important role in skin physiology. It may:
- Reduce sebaceous gland activity
- Increase sex hormone-binding globulin (SHBG), which lowers free testosterone
- Support hydration and skin barrier function
By increasing SHBG, estrogen may reduce circulating androgens that contribute to oil production.
In women with lower estrogen levels, providers may consider estrogen therapy as part of a broader plan.
Supporting Literature:
Hormonal correlates of acne and hirsutism.
Lucky, A. W. (1995). Hormonal correlates of acne and hirsutism. The American journal of medicine, 98(1), S89–S94.
Summary:
This review highlights how estrogen may counterbalance androgen effects and influence acne patterns in women.
Progesterone: Modulating Hormonal Fluctuations
Progesterone may:
- Influence sebaceous gland activity
- Interact with estrogen to maintain hormonal balance
- Contribute to cyclical acne patterns
Fluctuations — especially during the luteal phase — may correlate with breakouts.
In BHRT, progesterone is often used to support hormonal balance rather than directly address acne.
Supporting Literature:
Acne: hormonal concepts and therapy.
Thiboutot, D. (2004). Acne: hormonal concepts and therapy. Clinics in dermatology, 22(5), 419–428.
Summary:
This article discusses how hormone fluctuations, including progesterone, may influence acne severity.
Testosterone and Androgen Balance
Testosterone may:
- Increase sebum production
- Contribute to clogged pores
- Promote acne development
It is converted into DHT, a more potent androgen that strongly stimulates oil glands.
In BHRT, the focus is on balancing hormone levels, not simply increasing or decreasing testosterone.
Supporting Literature:
Acne and sebaceous gland function
Zouboulis, C. C. (2009). Acne and sebaceous gland function. Clinical Dermatology, 22(5), 360–366.
Summary:
This paper confirms the role of androgens in sebaceous gland activity and acne development.
DHEA: A Precursor Hormone
DHEA converts into both estrogen and testosterone.
It may:
- Influence androgen activity
- Affect oil production
- Contribute to acne when elevated
Because of its broad effects, DHEA use requires careful evaluation.
Supporting Literature
An update on the role of the sebaceous gland in the pathogenesis of acne
Makrantonaki, E., Ganceviciene, R., & Zouboulis, C. C. (2011). An update on the role of the sebaceous gland in the pathogenesis of acne. Dermato-endocrinology, 3(1), 41–49.
Summary:
The study suggests that because DHEA can be converted within the skin into more active androgens that influence oil production, individualized approaches — such as compounded DHEA when clinically appropriate — may be considered by providers as part of a broader hormone-balancing strategy for hormonal acne.
BHRT Dosage Forms for Hormonal Acne
Bioidentical hormone replacement therapy (BHRT) is often customized not only in hormone selection and strength, but also in dosage form. The way a hormone is delivered may influence how it is absorbed, metabolized, and tolerated. For patients with hormonally influenced acne, providers may select a dosage form based on individual hormone patterns, skin sensitivity, and overall therapy goals.
Topical Creams and Gels
Topical BHRT is one of the most commonly used approaches in compounding. These formulations are applied to the skin and absorbed transdermally.
- May allow for steady absorption of hormones into systemic circulation
- Often used for hormones such as estrogen, progesterone, or testosterone
- May be preferred for patients who want to avoid oral therapy
- Formulations can be adjusted for sensitive skin or specific application sites
Because hormonal acne involves the skin, some providers may consider topical delivery as part of a broader plan. Although, its primary role is systemic hormone support rather than direct acne therapy.

Oral Capsules
Compounded oral capsules are another common dosage form for BHRT.
- Typically used for progesterone or combination hormone therapies
- Undergo first-pass metabolism in the liver, which may influence hormone levels differently compared to topical forms
- May be preferred for patients who are already taking oral medications or prefer a familiar route
Oral dosing may be selected when systemic hormone regulation is the primary goal.
Sublingual Troches (Lozenges)
Troches are designed to dissolve under the tongue or in the cheek.
- Allow hormones to be absorbed through the oral mucosa, potentially bypassing some liver metabolism
- Often used for combination BHRT formulations
- May provide more flexible dosing and customization
This dosage form may be helpful when providers want more direct systemic absorption with adjustable dosing.
Vaginal Preparations
Vaginal creams or suppositories are sometimes used in BHRT, particularly for estrogen or DHEA.
- Provide localized hormone delivery
- Commonly used in menopausal care
- May contribute to overall hormone balance, which could indirectly influence acne patterns
These are typically used when other symptoms of hormone imbalance are also present.
Customized Combination Forms
One of the key advantages of compounding is the ability to combine multiple hormones into a single dosage form.
- May include combinations such as estrogen + progesterone
- Can be tailored in specific ratios and strengths
- May simplify regimens
This flexibility allows providers to design therapies based on individual hormone testing results and clinical presentation.
There is no single “best” dosage form for BHRT in hormonal acne. The choice depends on the patient’s hormone profile, preferences, and provider guidance. By offering multiple delivery options, compounding allows for a more individualized approach that may support broader hormone balance as part of an acne management plan.
The Role of Hormone Testing
Before considering therapies like BHRT, providers may recommend hormone testing to better understand what is happening internally.
Hormone testing may include:
- Estrogen (estradiol)
- Progesterone
- Testosterone
- DHEA
- Cortisol (in some cases)
These tests may be performed through:
- Saliva testing
- Blood spot testing
- Combination profiles
Testing provides insight into:
- Hormonal imbalances
- Patterns of estrogen or androgen dominance
- Fluctuations that may correlate with acne cycles
By identifying these patterns, providers can make more informed decisions about whether hormone-based therapies may be appropriate.
Personalized Hormone Consultations
Interpreting hormone levels and symptoms requires clinical context. For this reason, some patients may benefit from private hormone consultations with a trained professional.
Working with a hormone expert and compounding pharmacist — such as Lucy Andrews, PharmD — may provide:
- A detailed review of hormone test results
- Discussion of symptoms, including acne patterns
- Education on how hormones may be influencing skin health
- Collaboration with the prescribing provider on potential options
This type of consultation focuses on helping patients and providers better understand the connection between hormone balance and skin concerns.

Get to know your pharmacist
Lucy Andrews, PharmD
Pharmacist & Hormone Consultant
Lucy earned her Doctor of Pharmacy from The Ohio State University College of Pharmacy and has specialized in compounding since 2019. She focuses on hormone replacement therapy, women’s health, and nutritional supplements.
In 2023, she earned her certification in Hormone Replacement Therapy from The Professional Compounding Centers of America and actively attends conferences to expand her expertise. Lucy is passionate about personalized medicine, particularly in menopause management.
She values the ability to tailor hormone therapies to each patient’s unique needs, helping them regain confidence and improve their well-being during this major life transition. As both a compounding and consultant pharmacist, Lucy integrates her clinical knowledge with patient-centered care to provide customized solutions. Outside of work, she enjoys cooking, riding horses, and spending time with her family.
Where Dermatology Compounding Still Fits In
While BHRT addresses internal balance, topical options remain important.
Common compounded dermatology options may include:
- Spironolactone formulations
- Tretinoin combinations
- Clindamycin-based therapies
- Multi-ingredient acne creams
These target acne directly at the skin level and may be used alongside hormone-focused approaches. We are Ohio’s experts in BHRT as well as compounded dermatological therapies. Contact our pharmacy for step-by-step guidance through your skin care journey.

Central Ohio’s Trusted Hormone & Dermatology Compounding Pharmacy
At Central Ohio Compounding Pharmacy, we uphold strict standards and precise processes to support patient safety, comfort, and health goals.
We follow United States Pharmacopeia standards, including USP <795> and USP <797> , for consistent, accurate, and compliant preparations.
For every medication we prepare, we use pharmaceutical-grade ingredients from trusted suppliers and perform stability and potency checks to confirm each preparation meets expectations.
Your Partner in Hormonal Acne Support
Central Ohio Compounding Pharmacy is ready to support patients and providers seeking personalized solutions for hormonal acne — from compounded spironolactone to custom clindamycin gels. Every formulation we prepare is crafted with patient comfort and clinical goals in mind.
If you’re a patient, speak with your dermatologist or contact Central Ohio Compounding Pharmacy to explore custom options that fit your condition or lifestyle.
For Ohio dermatologists and prescribers, reach out to us to offer patients more personalized acne support options — proudly serving the communities of Worthington, Columbus, and Shipping throughout Ohio with valid prescription.
Contact Central Ohio Compounding Pharmacy to learn how personalized formulations may fit into your care plan.
References
- Da Cunha, M. G., Fonseca, F. L. A., & Machado, C. D. a. S. (2013). Androgenic Hormone Profile of Adult Women with Acne. Dermatology, 226(2), 167–171. Link
- Fox, L., Csongradi, C., Aucamp, M., Du Plessis, J., & Gerber, M. (2016). Treatment modalities for acne. Molecules, 21(8), 1063. Link
- Hormonal acne. (2025, July 18). Cleveland Clinic. Link
- Lucky, A. W. (1995). Hormonal correlates of acne and hirsutism. The American journal of medicine, 98(1), S89-S94. Link
- Makrantonaki, E., Ganceviciene, R., & Zouboulis, C. C. (2011). An update on the role of the sebaceous gland in the pathogenesis of acne. Dermato-endocrinology, 3(1), 41-49. Link
- Stubborn acne? Hormonal therapy may help. (n.d.-b). Link
- Thiboutot, D. (2004). Acne: hormonal concepts and therapy. Clinics in dermatology, 22(5), 419-428. Link
- Uysal, G., Sahin, Y., Unluhizarci, K., Ferahbas, A., Uludag, S. Z., Aygen, E., & Kelestimur, F. (2017). Is acne a sign of androgen excess disorder or not? European Journal of Obstetrics & Gynecology and Reproductive Biology, 211, 21–25. Link
- Zouboulis, C. C. (2004). Acne and sebaceous gland function. Clinics in dermatology, 22(5), 360-366. Link