BHRT BLOG SERIES
Navigating Hormonal Changes: Personalized Options for Women’s Wellness
Hormonal shifts during perimenopause and menopause can affect nearly every aspect of a woman’s physical and emotional well-being—from sleep quality and mood regulation to energy levels, sexual health, and joint health. While mass-produced, commercial therapies are widely used, many women and their healthcare providers are exploring more personalized, compounded options to manage these changes more effectively.
This blog series offers an educational look at bioidentical hormone replacement therapy (BHRT) from a compounding pharmacy perspective, focusing on specific medications and how they may be used to support women’s wellness. Each part of the series highlights a unique compounded hormone replacement therapy—explaining its form, common dosing, and clinical considerations—to help patients and providers understand what’s possible when care is individualized.
In Part 1 of our BHRT series, we introduced oral progesterone SR capsules and their potential role in supporting sleep and mood—particularly for women navigating perimenopause or menopause.
Part 2: Progesterone Cream: A Topical Approach to Hormonal Balance
Now in Part 2, we shift focus to another widely used form: topical progesterone cream. Unlike oral progesterone, which is metabolized through the liver and may produce calming metabolites, topical progesterone cream is absorbed through the skin and may offer more direct support for hormone balance and PMS symptoms without the sedating effects. Understanding these differences helps clarify why healthcare providers may choose one form over the other based on a patient’s specific symptoms and treatment goals.
Let’s explore how topical progesterone cream works, how it differs from oral forms, and the clinical evidence supporting its role in women’s hormonal health.
“We believe that topical progesterone is well absorbed and should be considered as an effective means of treating clinical conditions that respond favorably to progestogens.”
Source: Menopause
What are Compounded Progesterone Creams?
A compounded progesterone cream is a prescription medication that is custom-made by a compounding pharmacy to meet a patient’s specific hormonal needs. Unlike mass-produced, over-the-counter creams, compounded creams are prepared using pharmaceutical-grade ingredients in precise strengths and formulations as directed by a healthcare provider. This customization allows for adjustments in dose, absorption rate, and inactive ingredients, which can be especially helpful for patients who have sensitivities, require non-standard dosages, or need alternative application methods.
Because these products are not one-size-fits-all, they are formulated based on individual hormone levels, symptoms, and treatment goals—allowing providers to create a more personalized approach to hormone support.
If your aim is a personalized care plan in your journey through menopause, compounded progesterone creams are available in various strengths as well as custom strengths as needed (40mg/mL, 60mg/mL, 80mg/mL, 100mg/mL). Practitioners and pharmacists work together to assess each patient’s hormone levels, symptoms, and other factors to decide the appropriate dosage strengths. The prescription creams are dispensed in Topiclick cream dispensers (0.25mL = 1 click) for precise, pre-measured doses. This way, you can meet your dose schedule consistently.
How Progesterone Cream Works The Body
Mechanism of Action of Progesterone Cream
- Transdermal Absorption
- When applied to the skin, progesterone cream allows the hormone to be absorbed into the subcutaneous fat.
- From there, a portion of the hormone enters the systemic circulation.
- Binding to Progesterone Receptors
- Once in circulation, progesterone binds to intracellular progesterone receptors (PR-A and PR-B) located in tissues such as:
- Brain
- Endometrium (uterine lining)
- Breast tissue
- Bone
- Skin
- Once in circulation, progesterone binds to intracellular progesterone receptors (PR-A and PR-B) located in tissues such as:
- Gene Expression Modulation
- After binding to its receptor, the hormone-receptor complex moves into the cell nucleus, where it interacts with DNA to regulate the expression of target genes.
- This leads to cellular responses that influence menstrual cycle regulation, mood, sleep, and more.
- Neurosteroid Activity (limited with cream)
Unlike oral progesterone, topical progesterone is not significantly metabolized by the liver, so it produces fewer sedating neuroactive metabolites like allopregnanolone, which modulate GABA receptors in the brain.
Prescription progesterone cream may be prescribed during menopause or perimenopause for symptoms such as:
- Hot flashes
- Night sweats
- Perimenopausal cycle irregularity
- Breast tenderness
- Changes in skin elasticity
- Loss of firmness or thinning skin
- Increased appearance of fine lines or wrinkles
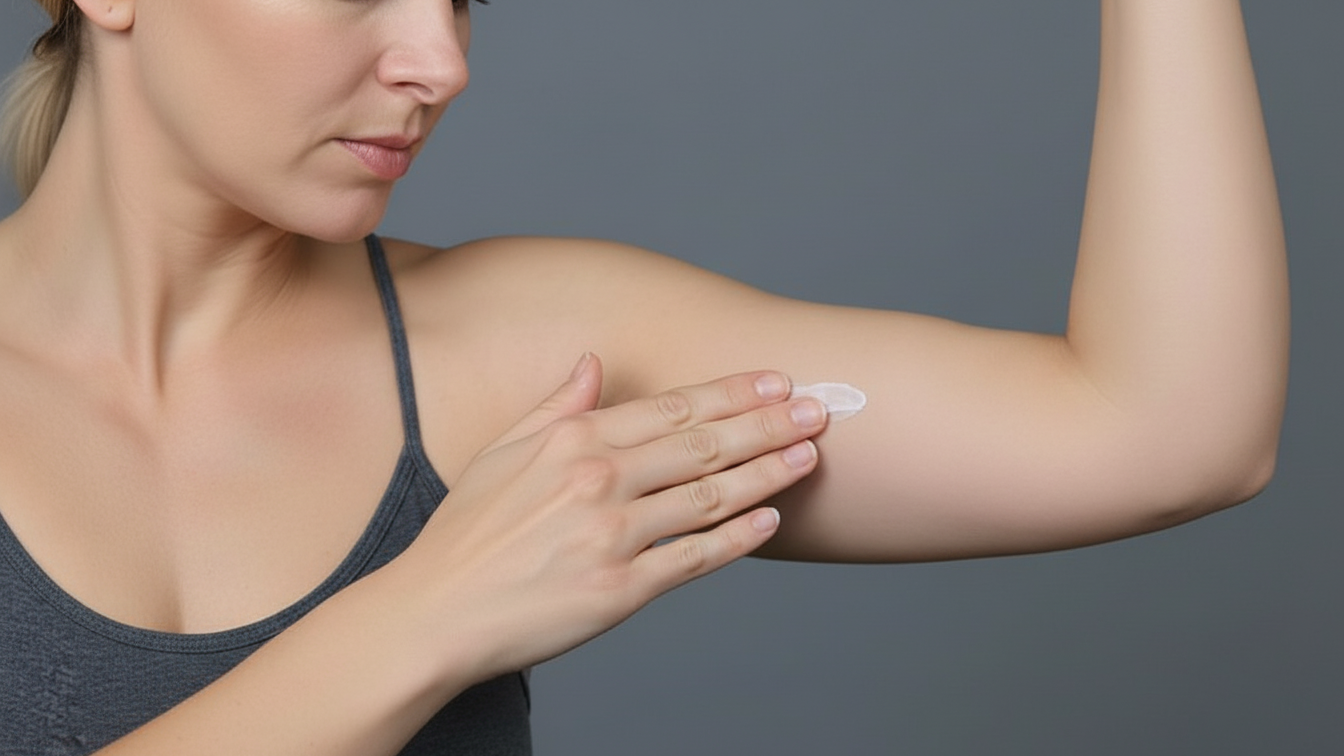
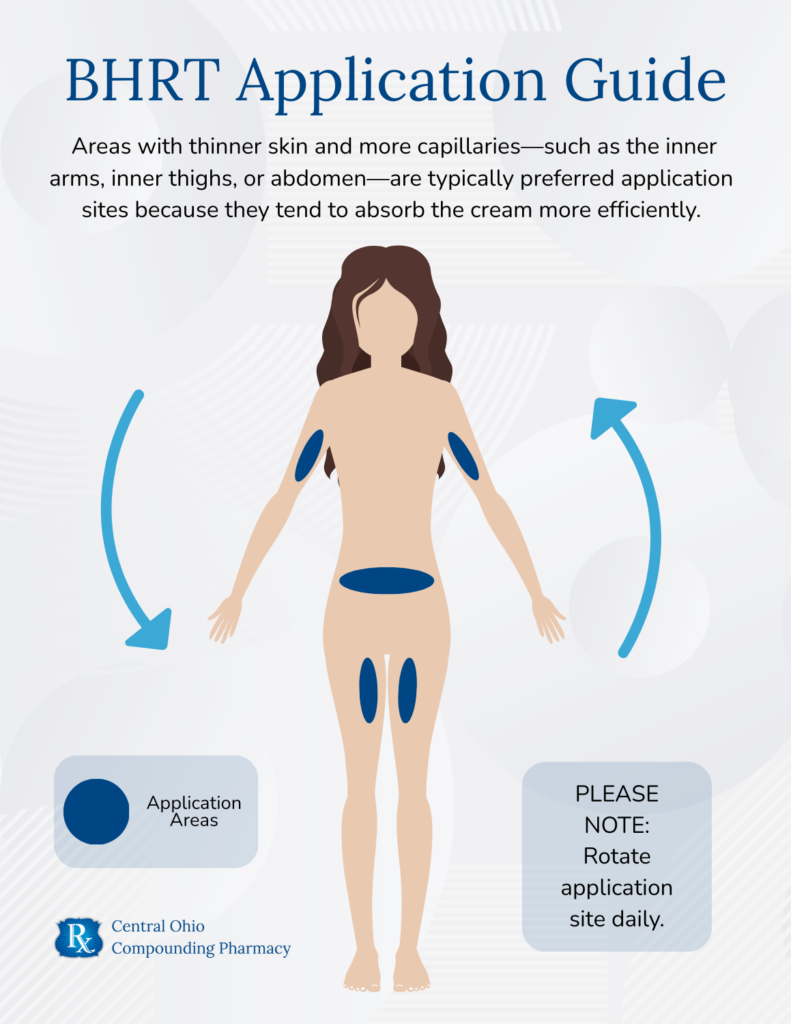
Why the Area of Application Matters for Progesterone Cream
Where you apply a compounded progesterone cream on the body can significantly impact how well the hormone is absorbed and how consistently it enters the bloodstream. That’s because skin thickness, blood flow, and fat content vary by body region, and these factors influence transdermal absorption.
For example, areas with thinner skin and more capillaries—such as the inner arms, inner thighs, abdomen, or behind the knees—are typically preferred application sites because they tend to absorb the cream more efficiently.
Rotating between recommended areas may help prevent skin irritation or buildup.
Applying progesterone to areas with thick skin or high fat content (like the soles of the feet or outer thighs) may reduce absorption and limit effectiveness.
For best results, patients should follow their provider’s instructions closely and avoid applying the cream over areas with broken or irritated skin, heavy lotions, or oils, as these can interfere with absorption.
Clinical Studies on the Use of Topical Progesterone Cream
Peer-reviewed studies highlighted the influence of progesterone creams in menopausal symptoms in women.
A study in Obstetrics and Gynecology randomly assigned 102 healthy women within five years of menopause to transdermal progesterone cream or placebo. Researchers evaluated various relevant factors, including complete history and serum studies. In the subject group, they found that 83% of women reported improvements in vasomotor symptoms, which include hot flashes and night sweats.
Another study in Fertility and Sterility explored how progesterone cream would help participants who showed signs of uterine overgrowth due to estrogen therapy. Their findings suggested that the topical route slowed the proliferation. Meaning, progesterone cream may provide support in uterine health.
Additionally, progesterone creams were assessed in peri‐ and postmenopausal-linked aging. Published in the British Journal of Dermatology, researchers evaluated the therapy’s influence on women’s skin. They monitored and assessed several measures, including skin elasticity and epidermal hydration. Results demonstrated the increase in elastic skin properties among the subjects, measured in three skin elasticity parameters. These suggested that progesterone creams might help with skin firmness, skin hydration, and skin wrinkles.
When Compounded Progesterone Cream May Provide Support for Women in Perimenopause or Menopause
For Patients
- Lena, 47:
Lena notices that hot flashes strike unpredictably throughout the day and disrupt her sleep at night. She prefers to avoid oral hormones because they make her feel groggy, and OTC progesterone creams don’t provide the consistent results she wants. Her provider recommends a compounded progesterone cream in a custom strength that allows her to apply a steady, skin-absorbed dose each evening. - Marisol, 51:
Marisol feels her skin has become thinner and less elastic since entering menopause, and she has also started experiencing mild night sweats. After trying several cosmetic products without improvement, she and her provider explore a compounded progesterone cream in a concentration that provides support without requiring a large amount of daily application. They choose a higher-strength option in 80 mg/mL, so she is applying a smaller amount of cream while still getting the amount of progesterone her provider recommends. The cream is dispensed in a metered click pump, giving her a precise 0.25 mL with each click, helping her to be consistent nightly. - Jessica, 45:
Jessica, a 45-year-old woman experiencing irregular periods, heightened anxiety, and breast tenderness visits her provider for help managing her symptoms. She completes a saliva hormone test, which reveals low progesterone levels in the luteal phase while estrogen remains within the normal range — a pattern consistent with estrogen dominance. Since she’s still menstruating and prefers a non-oral, bioidentical option, her provider suggests using progesterone cream during the second half of her cycle (days 14–28). The goal is to help balance her estrogen levels, support mood stability, and potentially reduce breast discomfort. A follow-up is scheduled in two months to reassess symptoms and determine if dosage adjustments are needed.
For Providers
- A clinician working with a patient experiencing vasomotor symptoms who prefers non-oral delivery may choose a compounded progesterone cream to offer a gentle, transdermal option with flexible dosing.
- Gynecologists managing patients with sensitivities to commercial or cosmetic-grade ingredients may find compounded progesterone cream helpful, as it can be prepared in allergen-free or fragrance-free bases.
Functional and integrative practitioners may incorporate compounded progesterone cream into individualized BHRT plans, adjusting strength and application schedules based on lab values, symptom tracking, and patient response.
Considering Whether Topical Progesterone Cream Is Right for You
Your transition into perimenopause or menopause doesn’t happen all at once. It shows up in little ways until you sense that something feels off. If you’re searching for a gentle way to support your body, topical progesterone cream may be one option worth exploring.
Compared to one-size-fits-all, mass-produced commercially available medications, compounded medications are flexible/customizable in dosing and formulation. Some women may respond well to 40mg/mL, while others may feel comfort at 100mg/mL. At any point of your journey, that flexibility lets your doctor adjust the dose as needed.
Our pharmacists at Central Ohio Compounding Pharmacy are here to support that conversation, help you understand options, and work with your provider to find the optimal approach for your well-being. Since BHRT uses bioidentical hormones, the active ingredient in compounded progesterone creams match the progesterone your body naturally produces, potentially supporting tolerability.
Consult your healthcare provider or pharmacist to check your hormone levels and help you figure out the best care plan for you. Compounded therapy is highly personalized and should be clinically guided by a prescriber with experience in hormone health.
Lucy Andrews, PharmD
Please schedule a virtual or in-person consultation with our hormone specialist, Lucy Andrews, PharmD.
We also offer educational resources to support informed, evidence-based care.
Now is the perfect time to assess your hormone levels (at-home saliva test kits available) and discuss advanced options to gain balance, address specific symptoms, and enhance quality of life.
Talk to your healthcare provider about whether Hormone Replacement Therapy is appropriate for you based on your symptoms, age, and health history.
Need a Referral to a Trusted Women’s Health Practitioner?
Check out our list of Ohio practitioners we know and trust.
For Prescribers: Expanding Therapy Options
Clinicians looking to broaden their therapeutic options for women in perimenopause or menopause may find compounded topical progesterone creams to be a valuable addition to individualized care plans. This transdermal route offers an alternative for those who want to avoid oral formulations, certain excipients, or prefer a choice that integrates easily into routines.
With BHRT, providers may elevate their practice through personalized options that meet their patients’ specific needs, symptoms, and preferences. We’re here to support you with customized approaches that align with the most current clinical standards. Please don’t hesitate to reach out with questions or for support in discussing next steps.
How to Prescribe: Central Ohio Compounding Pharmacy RX Order Forms
To make the prescribing process simple, Central Ohio Compounding Pharmacy provides an easy-to-use RX order form listing all available strengths of topical compounded progesterone creams, as well as other BHRT options. Prescribers can simply check the desired strength (40mg/mL, 60mg/mL, 80mg/mL, 100mg/mL, or custom) and quantity (7.5mL, 15mL, 22.5mL, 30mL, custom mL), then fax in the form directly to the pharmacy.
This streamlined process ensures accuracy, convenience, and quick turnaround times for both patients and providers.
In the News: Updated FDA Guidance on Hormone Therapy
Recently, the FDA updated its labelling requirements by removing the black box warning from hormone therapy medications. This change is based on newer research and expert review showing that hormone therapy, when appropriately prescribed, is safe and may show potential in supporting women and their health.
Stay Tuned for the Next Installment in Our BHRT Blog Series
Coming Soon: Part 3 — Estriol/Estradiol Vaginal Cream for Vaginal Atrophy and Dryness
In Part 3 of our BHRT Menopause Series, we’ll explore topical estriol/estradiol cream and how it differs from oral forms in terms of delivery, metabolism, and symptom relief.
COMING UP NEXT
Part 3: Estriol/Estradiol Vaginal Cream for Vaginal Atrophy and Dryness
Part 4: Testosterone Vaginal Cream for Energy, Libido, and Tissue Health
Part 5: DHEA Vaginal Gel: A Compounded Option for Vaginal Dryness and Hormonal Support
Part 6: Topical Testosterone Cream for Women: A Personalized Approach to Hormonal Wellness
References
- Du, J. Y., Sanchez, P., Kim, L., Azen, C. G., Zava, D. T., & Stanczyk, F. Z. (2013b). Percutaneous progesterone delivery via cream or gel application in postmenopausal women. Menopause the Journal of the North American Menopause Society, 20(11), 1169–1175. Link
- Holzer, G., Riegler, E., Hönigsmann, H., Farokhnia, S., & Schmidt, B. (2005b). Effects and side-effects of 2% progesterone cream on the skin of peri- and postmenopausal women: results from a double-blind, vehicle-controlled, randomized study. British Journal of Dermatology, 153(3), 626–634. Link
- Leonetti, H. B., Longo, S., & Anasti, J. N. (1999b). Transdermal progesterone cream for vasomotor symptoms and postmenopausal bone loss. Obstetrics and Gynecology, 94(2), 225–228. Link
- Leonetti, H. B., Wilson, K., & Anasti, J. N. (2003b). Topical progesterone cream has an antiproliferative effect on estrogen-stimulated endometrium. Fertility and Sterility, 79(1), 221–222. Link